Imagine a world where one of the most commonly prescribed pain relievers, found in medicine cabinets across the globe, has a secret. A mechanism of action (MoA) that, until recently, was largely unknown to the medical community. This is not science fiction, but the reality of paracetamol (also known as acetaminophen).
Paracetamol: A Household Name with a Hidden Mechanism
Paracetamol, a staple in the World Health Organization’s List of Essential Medicines, has been a go-to analgesic for decades. Its safety profile and efficacy in managing mild to moderate pain have made it a favorite among healthcare professionals worldwide. But here’s the kicker: recent research has unveiled that paracetamol’s pain-relieving effects are intricately linked to the Endocannabinoid System (ECS).
The ECS Connection: A Paradigm Shift
The discovery that paracetamol’s analgesic effects involve the ECS is nothing short of revolutionary. This finding not only sheds light on the drug’s mechanism of action but also underscores the critical importance of the ECS in pain modulation .
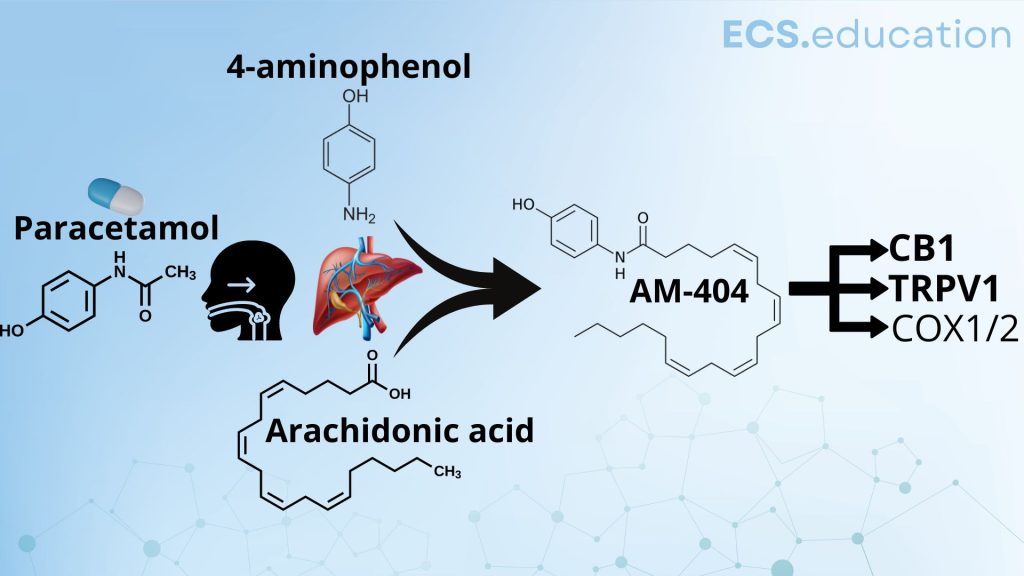
Here’s how it works: Paracetamol is metabolized to p-aminophenol in the liver, which gets fused to arachidonic acid to form AM404, a compound that inhibits the reuptake of the endocannabinoid anandamide and activates TRPV1. This leads to increased levels of anandamide in the synaptic cleft, enhancing its pain-relieving effects. In essence, paracetamol indirectly activates the ECS to alleviate pain.
The Irony of Medical Education
Despite this groundbreaking discovery, the ECS remains conspicuously absent from medical curricula and textbooks worldwide. Our previous analysis of the Guyton and Hall Textbook of Medical Physiology revealed a complete omission of the ECS, even in its 2020 edition. This oversight extends to the mechanism of action of paracetamol, a drug that countless doctors prescribe daily.
The implications are profound:
- Incomplete Understanding: Physicians recommending paracetamol may not fully grasp its mechanism of action.
- Missed Opportunities: The ECS’s role in pain management remains underexplored in clinical practice.
- Patient Care Impact: A comprehensive understanding of paracetamol’s MoA could inform more effective pain management strategies.
A Call to Action for Medical Education
The paracetamol-ECS connection serves as a powerful argument for the inclusion of ECS education in medical curricula:
- Relevance: Understanding the ECS is crucial for comprehending the action of one of the world’s most prescribed medications.
- Patient Safety: Knowledge of the ECS could inform better pain management strategies and potential drug interactions.
- Scientific Integrity: Medical education should reflect current scientific understanding, including the role of the ECS in physiological processes.
Conclusion: Bridging the Knowledge Gap
The revelation of paracetamol’s connection to the ECS is a wake-up call for the medical community. It highlights a critical gap in our understanding of both a widely used medication and a fundamental physiological system.
As we’ve previously reported, up to 95% of physicians worldwide report inadequate knowledge about medical cannabis and, by extension, the ECS . This statistic becomes even more alarming when we consider that many of these same physicians regularly prescribe a drug that acts on this very system.
It’s time for medical education to catch up with scientific discovery. Every healthcare professional who recommends paracetamol should have a basic understanding of the ECS. This knowledge is not just academic; it’s essential for providing informed, effective patient care.
The paracetamol-ECS connection is more than a fascinating scientific tidbit—it’s a compelling reason to revolutionize medical education. Let’s ensure that the next generation of healthcare providers is equipped with a comprehensive understanding of the ECS, starting with the medications they prescribe every day.


Comments (2)
Comments are closed.